ACLS Tachycardia Algorithm
The ACLS Tachycardia Algorithm is used for patients who have marked tachycardia, usually greater than 150 beats per minute, and a palpable pulse.
Some patients may have cardiovascular instability with tachycardia at heart rate less than 150 bpm. It is important to consider the clinical context when treating adult tachycardia.
If a pulse cannot be felt after palpating for up to 10 seconds, move immediately to the ACLS Cardiac Arrest VTach and VFib Algorithm to provide treatment for pulseless ventricular tachycardia.
The immediate response to an adult patient with tachycardia and a palpable pulse is
- To maintain an open airway
- Assist breathing if necessary
- Apply monitors to assess cardiac rhythm, blood pressure, blood oxygenation
- Provide supplement oxygen to maintain O2 saturation between 94% and 99%
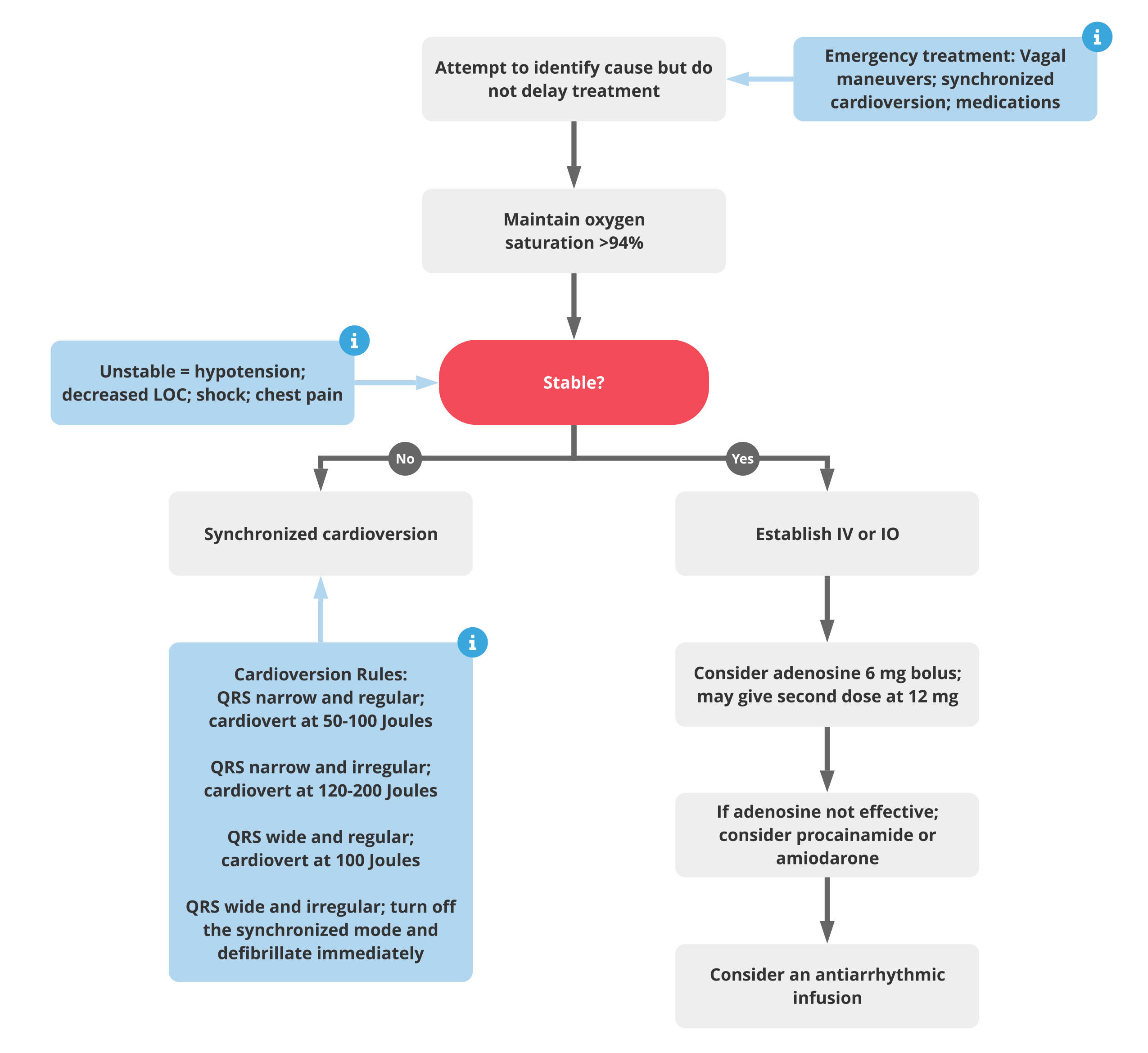
The main assessment in adult patients with tachycardia is to determine whether the patient is stable or not. Signs of cardiovascular instability are hypotension, signs of shock or acute heart failure (flash pulmonary edema, jugular venous distention), altered mental status, or ischemic chest pain.
Unstable patients with tachycardia should be treated with synchronized cardioversion as soon as possible.
|
Cardioversion Rules |
|
| QRS narrow and regular | 50-100 Joules |
| QRS narrow and irregular | 120-200 Joules |
| QRS wide and regular | 100 Joules |
| QRS wide and irregular | Turn off the synchronized mode and defibrillate immediately |
Stable patients with tachycardia with a palpable pulse can be treated with more conservative measures first.
- Attempt vagal maneuvers
- If unsuccessful, administer adenosine 6 mg IV bolus followed by a rapid normal saline flush
- If unsuccessful, administer adenosine 12 mg IV bolus followed by a rapid normal saline flush
- Beta-blockers and calcium channel blockers may be considered for narrow QRS tachycardia (QRS <0.12 sec)
- For stable, wide QRS complex tachycardia (QRS ≥0.12 sec)
- Strongly consider expert consultation
- Consider procainamide 20-50 mg/min IV, OR
- Amiodarone 150 mg IV over 10 minutes, OR
- Sotalol 100 mg (1.5 mg/kg) over 5 minutes