PALS Post Arrest Shock Management Algorithm
After successful resuscitation, the team must continue to manage the airway, ventilation, and circulation and perform diagnostic testing. Post-resuscitation measures should include:
- Treatment of the underlying causes of the initial injury or illness;
- Prevention of further injury; Optimization of body functions
- Transport to the next level of care
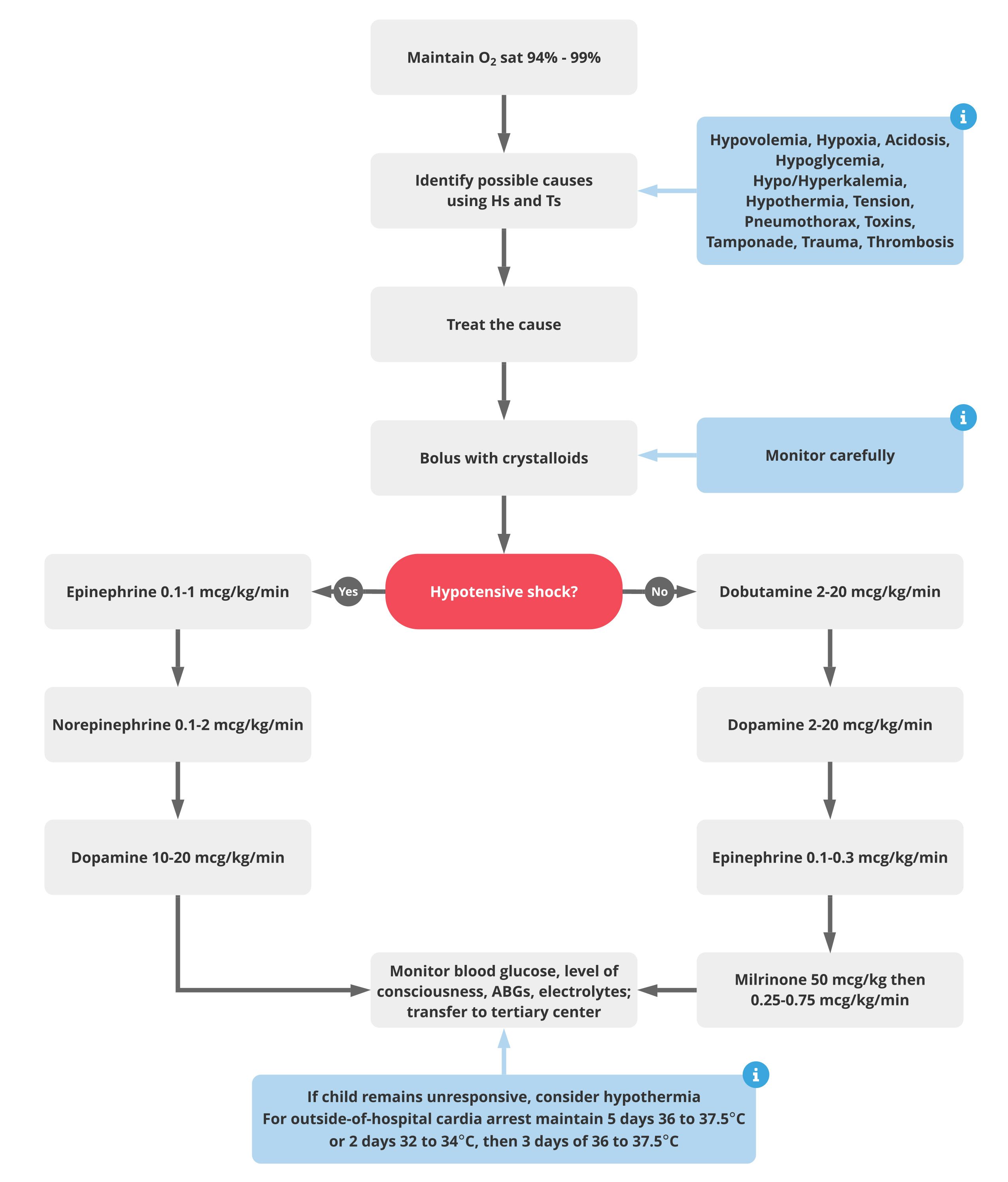
To meet these goals, rescuers should focus on respiratory, cardiovascular, neurologic, renal, gastrointestinal, and hematologic systems. Administer oxygen as needed in order to maintain a blood oxygenation level/saturation greater than 94% (based on pulse oximetry). If the precise cause of the initial shock symptoms has not yet been identified, consider possible causes of shock in the pediatric patient.
It is often helpful to remember the H’s and the T’s:
- Hypovolemia
- Hypoxia
- (H+) Acidosis
- Hypoglycemia
- Hypo/Hyperkalemia
- Hypothermia
- Tension Pneumothorax
- Toxins
- Tamponade
- Trauma
- Thrombosis
Once the cause has been identified, provide definitive treatment as soon as possible. It will usually also be necessary to provide additional fluid boluses. When needed, give crystalloid for volume resuscitation. Monitor fluid resuscitation carefully.
Volume resuscitation may not be enough to maintain the child's blood pressure. In these cases, you may consider adding pressors. One approach is to start with epinephrine, then move to norepinephrine, then move to dopamine. Alternatively, some rescuers will begin with dobutamine, then progress to dopamine, then try epinephrine followed by milrinone. The doses of these cardiovascular agents are based on the size of the patient and then titrated to maintain an effective blood pressure. These agents require an intensive care unit, an arterial line, and constant monitoring. Diagnostic tests should be done at the same time as interventions.
For cardiac arrest outside of hospital, start and maintain targeted temperature management:
- 5 days at 36°C to 37.5°C OR
- 2 days at 32°C to 34°C followed by 3 days at 36°C to 37.5°C